Introduction
In the vast ecosystem of microorganisms that inhabit the human body, Candida occupies a unique and sometimes troublesome position. While it is a natural part of our microbiota, certain conditions allow it to grow unchecked, leading to infections commonly referred to as candidiasis. For decades, scientists, doctors, and nutritionists have studied Candida not only as a medical concern but also as a fascinating example of how delicate the balance between microorganisms and human health can be.
This article explores what Candida is, why it matters, how it causes problems, and what can be done to prevent and treat related conditions.
What is Candida?
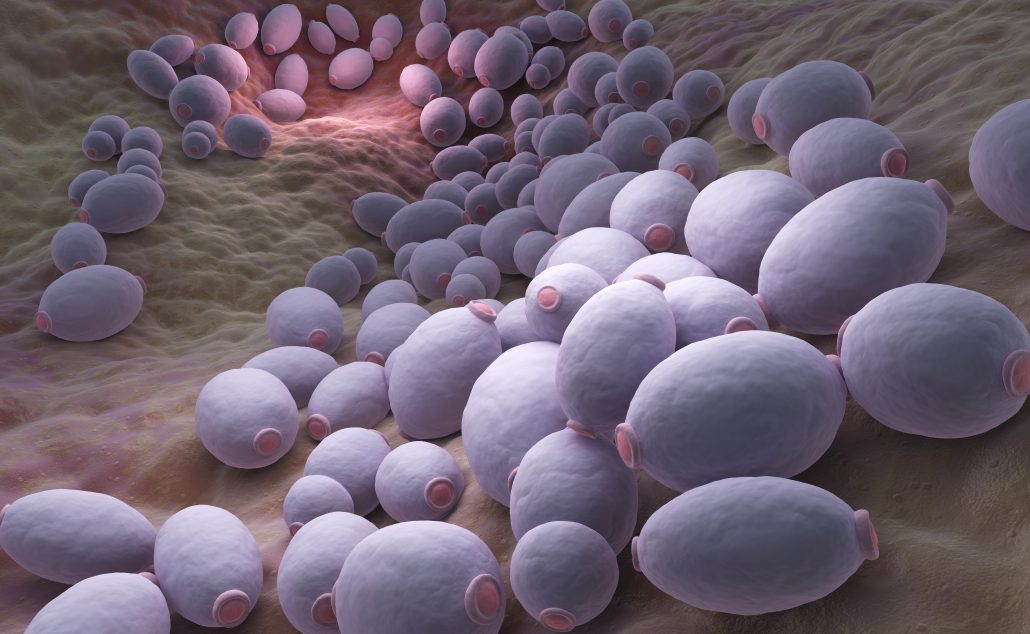
Candida is a genus of yeasts (fungi) that live in various parts of the human body. Among its many species, Candida albicans is the most common and clinically significant. Others, such as Candida glabrata, Candida tropicalis, and Candida krusei, are also medically relevant, especially in people with weakened immune systems.
Normally, Candida exists in small amounts in the mouth, gut, vagina, and skin, coexisting harmlessly with other microorganisms. It only becomes problematic when environmental factors—such as antibiotics, high sugar intake, weakened immunity, or hormonal changes—disturb the balance of the body’s microbiome, allowing yeast to overgrow.
Types of Candida Infections
Candida infections are diverse and affect different parts of the body:
-
Oral Thrush – A white, creamy coating inside the mouth, often accompanied by soreness. It is common in infants, denture wearers, and individuals on antibiotics or corticosteroids.
-
Vaginal Yeast Infection – Perhaps the most well-known manifestation, characterized by itching, burning, abnormal discharge, and discomfort. Hormonal changes, tight clothing, and antibiotic use can increase the risk.
-
Cutaneous Candidiasis – Skin infections that thrive in warm, moist areas like armpits, groin, and folds of skin, producing red rashes and itching.
-
Invasive Candidiasis – The most serious form, where Candida enters the bloodstream or internal organs. This life-threatening condition mainly affects hospitalized or immunocompromised individuals, such as cancer or HIV patients.
Risk Factors for Candida Overgrowth
Not everyone develops candidiasis, but certain factors significantly increase susceptibility:
-
Antibiotic use – Broad-spectrum antibiotics kill beneficial bacteria, giving Candida room to flourish.
-
High sugar diets – Yeast thrives on glucose, making diets rich in sugar and refined carbs a risk factor.
-
Hormonal changes – Pregnancy, oral contraceptives, and hormone replacement therapies can alter vaginal pH and microbiota.
-
Weakened immunity – HIV/AIDS, chemotherapy, or organ transplantation leave individuals vulnerable.
-
Medical devices – Catheters, IV lines, and dentures provide surfaces for Candida biofilms to form.
Symptoms and Diagnosis
The symptoms of candidiasis vary depending on the type of infection:
-
Oral thrush: white patches, loss of taste, pain while eating.
-
Vaginal yeast infection: itching, burning, swelling, thick discharge resembling cottage cheese.
-
Skin infection: redness, itching, pustules.
-
Invasive candidiasis: fever, chills, and sepsis-like symptoms that do not improve with antibiotics.
Diagnosis usually involves a physical examination, microscopic analysis of samples, or cultures to identify the yeast. Advanced blood tests and molecular methods may be necessary in severe cases.
Treatments for Candida Infections
Treatment depends on the infection site and severity.
-
Topical antifungals – Creams, ointments, and suppositories containing clotrimazole, miconazole, or nystatin are common for skin and vaginal infections.
-
Oral antifungals – Fluconazole and itraconazole are widely prescribed for more stubborn infections.
-
Intravenous antifungals – In cases of invasive candidiasis, echinocandins (like caspofungin) or amphotericin B may be administered in hospital settings.
-
Lifestyle adjustments – Reducing sugar intake, wearing breathable fabrics, and practicing good hygiene help prevent recurrences.
The Role of Diet and Lifestyle
There is growing interest in the relationship between Candida and diet. While some alternative health sources promote the “Candida diet”—which eliminates sugars, alcohol, refined carbs, and yeast-containing foods—the scientific evidence is mixed. However, there is consensus that limiting sugar and refined carbohydrates can support a healthier microbiome and discourage yeast overgrowth.
Probiotics, such as those found in yogurt or supplements, may also help restore microbial balance, though results vary among individuals. Stress management, exercise, and adequate sleep further strengthen the immune system, reducing susceptibility.
Candida and the Human Microbiome
The story of Candida is also a story about the microbiome. In healthy individuals, bacterial populations—especially Lactobacillus species in the gut and vagina—keep Candida in check. When this balance is disrupted, yeast gains the upper hand.
Modern research is uncovering fascinating connections between Candida and chronic conditions. Some studies suggest that Candida overgrowth may be linked to gastrointestinal disorders, autoimmune conditions, and even mood changes, though causation remains unclear. This area of study is still emerging but offers exciting possibilities for personalized medicine.
Misconceptions About Candida
Because candidiasis is common and uncomfortable, myths abound:
-
Myth 1: Only women get yeast infections.
In reality, men can also develop genital candidiasis, though less frequently. -
Myth 2: Candida diets cure everything.
While diet influences yeast growth, extreme restrictions are not universally supported by science. -
Myth 3: Over-the-counter creams always work.
Some strains of Candida are resistant to common antifungals, requiring prescription treatment. -
Myth 4: Candida is always harmful.
Candida is part of the natural flora; problems arise only when overgrowth occurs.
Prevention Strategies
Preventing candidiasis involves a combination of medical awareness and lifestyle choices:
-
Use antibiotics only when prescribed and necessary.
-
Maintain good oral and genital hygiene.
-
Choose breathable clothing to reduce moisture.
-
Manage chronic health conditions like diabetes effectively.
-
Incorporate balanced nutrition to support a healthy microbiome.
Candida in a Global Health Context
Candida infections are not just personal inconveniences—they represent a public health challenge. Invasive candidiasis, in particular, causes hundreds of thousands of hospitalizations worldwide each year, with significant mortality rates. The rise of antifungal resistance further complicates treatment, echoing the global concern seen with antibiotic resistance.
Research into new antifungal drugs, vaccines, and microbiome-based therapies is ongoing, reflecting the medical community’s recognition of Candida as both a common and potentially dangerous pathogen.
Conclusion
Candida is a reminder of the fine line between harmony and disruption in the human body. As a natural inhabitant of our microbiota, it usually lives quietly, unnoticed. Yet when conditions tip in its favor, it can cause infections ranging from mild discomfort to life-threatening illness.
Understanding Candida requires a multifaceted approach—biological, medical, lifestyle, and public health. Awareness, proper diagnosis, responsible treatment, and prevention strategies can reduce its burden. And as research continues to uncover the complex interplay between Candida and human health, we gain not only better treatments but also deeper insights into the fragile ecosystems within us.